Neurological Symptoms: What They Mean and What To Do
A sudden numb arm, persistent tingling in your feet, or new, severe headaches can feel scary. Some neurological symptoms are temporary and harmless. Others need fast medical attention. This page helps you spot the difference, record useful details, and act quickly when it matters.
Common Symptoms and Likely Causes
Tingling, numbness, burning or a pins-and-needles feeling often points to nerve irritation. That can come from diabetes, vitamin deficiencies, nerve compression (like a pinched neck), or certain medications. Muscle weakness or loss of coordination can come from stroke, multiple sclerosis, or severe nerve damage. Dizziness, balance problems, and fainting may be inner-ear issues, dehydration, or neurological causes that need testing. New, sudden severe headache—especially with vomiting or neck stiffness—requires urgent evaluation.
Memory lapses or confusion that start suddenly are different from slow, gradual changes. Sudden changes suggest stroke or infection. Gradual problems may come from neurodegenerative conditions, medication side effects, metabolic issues, or long-term vascular disease.
What to Watch For — Red Flags
If you or someone near you has any of these, call emergency services or go to the ER right away: sudden weakness on one side of the body, slurred speech, sudden vision changes, severe sudden headache unlike previous ones, loss of consciousness, or sudden confusion. These are classic stroke or serious brain-event signs.
Other urgent but less dramatic signs include progressive weakness that gets worse over days, new seizures, high fever with neck stiffness and altered mental state, or trouble breathing due to a swallowing problem. Don’t wait for symptoms to resolve if they’re getting worse.
For non-urgent but worrying symptoms—mild ongoing numbness, chronic tingling, intermittent dizziness—book a primary care or neurology visit. Bring a timeline, a list of medications, and note what makes symptoms better or worse.
Medication-related neurological symptoms are common. Some drugs cause dizziness, tremor, or neuropathy. If you started a new medicine and notice new nerve symptoms, talk to your prescriber before stopping the drug. They may adjust the dose or switch treatments. Online pharmacy purchases should be from trusted sources and paired with medical advice.
Testing may include a focused neurological exam, blood tests (glucose, B12, thyroid), MRI or CT scans, and nerve studies (EMG, nerve conduction). These help pinpoint whether the problem is in the brain, spinal cord, nerves, or muscles.
Practical steps you can take now: keep a symptom diary with time, triggers, and severity; list all medications and supplements; control chronic risks like high blood sugar and high blood pressure; avoid alcohol and recreational drugs that can worsen symptoms. For persistent symptoms, ask for a neurology referral and bring notes to the appointment.
If you’re unsure how serious your symptom is, call a nurse line or your doctor for quick advice. Fast, clear information helps get the right care sooner—and that often changes outcomes for the better.
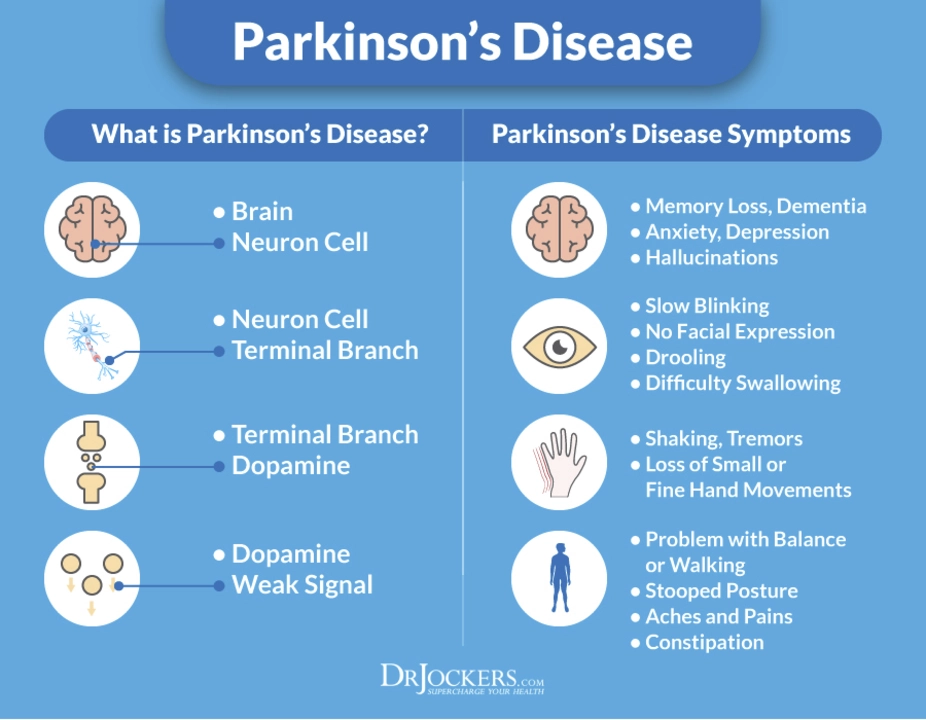
Understanding Clinically Isolated Syndrome: A Comprehensive Overview
In my latest blog post, I provided a comprehensive overview of Clinically Isolated Syndrome (CIS). This is a term used to describe the first neurological episode that may be indicative of Multiple Sclerosis (MS). In the post, I discussed the symptoms, diagnostic process, and treatment options for CIS. I also emphasized the importance of early intervention and close monitoring by healthcare professionals in the management of this condition. Overall, it's essential to understand CIS as it may be the first sign of a potentially life-altering disease, like MS.
View More