
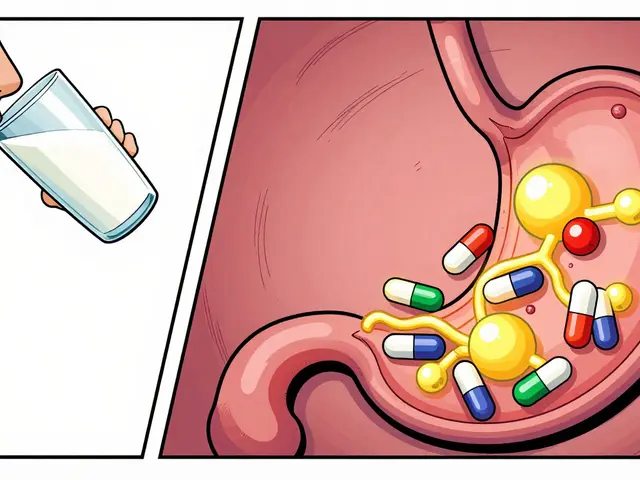
Every year, over 107,000 people in the U.S. die from drug overdoses. Many of these deaths aren’t caused by one drug alone-they happen when substances mix in dangerous ways. The biggest killers? Opioids combined with alcohol, benzodiazepines, or other central nervous system (CNS) depressants. These combinations don’t just add up-they multiply risk. A single pill of oxycodone might be manageable. Add a few sips of wine or a sleeping pill, and your breathing can slow to a stop without warning. The good news? 90% of these deaths are preventable if you know what to look for and how to check.
Why Some Drug Mixes Are Deadly
Not all drug interactions are the same. Some cause nausea or dizziness. Others can shut down your lungs. The most dangerous combinations all affect the same part of your brain: the area that controls breathing. Opioids like oxycodone, fentanyl, or heroin already slow breathing. When you add another depressant, your body loses its ability to keep oxygen flowing. This isn’t theoretical-it’s measurable. A 2022 study in JAMA Internal Medicine found that mixing opioids with benzodiazepines like Xanax or Valium increases the risk of fatal overdose by more than 10 times. Alcohol? That combo bumps up respiratory depression risk by 67%, according to NIH data from 2021.It’s not just prescription drugs. Street drugs are often laced with unknown substances. What someone thinks is heroin might be fentanyl-laced cocaine. What’s sold as Molly could be a synthetic opioid. These aren’t random accidents. They’re predictable outcomes of unmonitored polydrug use. The CDC reports that 75% of opioid-related overdoses involve multiple substances. And most people don’t realize they’re at risk because they think, “I only take one thing at a time.”
What Tools Exist to Check for Interactions
There are digital tools, but they have blind spots. The FDA’s Drug Interaction Checker, updated monthly, covers over 1,200 medications. MedlinePlus and Medscape’s tools are also reliable for prescription and OTC drugs. But here’s the problem: they don’t know what you’re not telling them. If you don’t mention alcohol, marijuana, or a pill you got from a friend, the app won’t warn you. A 2022 BMJ study found these tools catch only 76% of dangerous interactions when relying on patient reports. The real gap? Illicit drugs. Over 63% of dangerous interactions involve substances not listed in any database.That’s why clinical tools are better. The CDC’s Opioid Risk Tool (ORT) is a five-question screening used in doctor’s offices. It takes less than two minutes and has a 95% sensitivity for spotting misuse. But even this tool misses the real danger: non-prescribed use. That’s why experts say asking “Are you taking other medications?” is too vague. The right question is: “Do you ever take medicines not prescribed to you?” That simple shift increases honest answers by 52%, according to a 2022 study in Addiction.

How Harm Reduction Programs Do It Differently
In emergency rooms and community outreach programs, the approach is different. Instead of asking for drug names, they show a list of common substances. The National Harm Reduction Coalition’s “Overdose Risk Assessment Card” lists 23 items: alcohol, Xanax, Valium, sleeping pills, fentanyl, cocaine, meth, heroin, MDMA, and more. The question isn’t “Are you on any meds?” It’s: “Have you used any of these in the last week?”This method works because it removes stigma. People are more likely to admit to using Valium than to say they’re mixing it with painkillers. In fact, one ER nurse shared on Reddit that after 12 years of work, she saw 217 overdose cases where patients denied benzodiazepine use-until after naloxone was given. Then, 82% admitted they’d been mixing them. That’s the power of direct, non-judgmental questions.
Pharmacists are also key. The Beers Criteria, updated every two years by the American Geriatrics Society, lists 56 dangerous combinations for older adults. But even here, the biggest risk isn’t what’s prescribed-it’s what’s shared. Jarrod McMaugh from the Pharmaceutical Society of Australia pointed out that Real Time Prescription Monitoring systems only capture 37% of actual medications consumed because people share pills with family, friends, or partners. That’s why asking “Did anyone else give you this?” is just as important as checking the label.
What You Can Do Right Now
You don’t need a doctor or an app to protect yourself. Here’s what works:- Know the red flags: If you’re taking an opioid (even a low dose), avoid alcohol, sleeping pills, muscle relaxers, or anti-anxiety meds. Even one drink can be risky.
- Ask about street drugs: If you use substances outside prescriptions, assume they’re contaminated. Fentanyl is now found in nearly 70% of seized cocaine and meth samples. No app can warn you about that.
- Use the self-check tool: The National Harm Reduction Coalition offers a free “Overdose Risk Self-Check” online in 12 languages. It asks 10 simple questions based on clinical guidelines and is 88% accurate.
- Carry naloxone: If you or someone you know uses opioids or depressants, have naloxone on hand. It’s free at many pharmacies and community centers. It won’t stop an overdose from happening-but it can bring someone back.
- Learn street names: “Molly” could mean MDMA-or fentanyl. “Downers” might mean Xanax, Klonopin, or even a counterfeit opioid pill. Knowing these terms helps you ask better questions.

Why Most People Miss the Warning Signs
The biggest reason overdoses keep happening? People don’t realize they’re mixing. A 2023 SAMHSA survey found that 68% of people prescribed opioids were never asked about alcohol or benzodiazepine use. Another study showed that 58% of patients underreport benzodiazepine use because they think it’s not “real drug use.” But when you combine these with opioids, the risk isn’t just higher-it’s exponentially higher.Doctors and pharmacists are learning. In 2019, only 22% of U.S. hospitals asked about non-prescribed substances. By 2023, that number jumped to 63%. But outside clinical settings, support is still lacking. Only 17% of syringe service programs have access to pharmacists who can check interactions. That’s why community-based tools like the Overdose Risk Assessment Card are so vital. They fill the gap where the system fails.
What’s Changing in 2026
In February 2024, the FDA updated its Drug Interaction Checker to include data on 47 fentanyl analogs and 12 new synthetic opioids. That’s progress. But technology alone won’t save lives. The real breakthrough is in how we ask questions. Instead of “Are you taking other drugs?” the new standard is: “What have you taken in the last week-and who gave it to you?”AI is also being tested. A 2023 study in JAMA Internal Medicine showed machine learning could predict dangerous polydrug use from electronic records with 92% accuracy. But privacy concerns and bias in data mean these tools aren’t ready for prime time. The human connection still matters most.
The bottom line? Overdose risk isn’t about how much you take. It’s about what you mix. The most effective prevention isn’t a high-tech app or a complex medical test. It’s a simple conversation. One that’s honest. One that doesn’t judge. One that asks the right question at the right time.
11 Comments
Robert Bliss
March 10, 2026 at 13:43 PM
this hit hard. i carry naloxone in my pocket now. not because i use drugs, but because my cousin does. and if i can be the person who doesn’t panic and just hands over the shot? that’s worth it. simple. no drama. just life-saving. 🤝
Mantooth Lehto
March 11, 2026 at 13:27 PM
I can't believe people still think this is just about 'bad choices'-it's systemic. The system fails people at every level: doctors don't ask, pharmacies don't track, and the government still treats addiction like a moral failure. We need real harm reduction, not more stigma. And stop calling it 'drug abuse.' It's survival.
Samantha Fierro
March 12, 2026 at 21:10 PM
I work in an ER, and the shift in patient honesty after we started using the Overdose Risk Assessment Card was immediate. Before? 1 in 5 admitted to mixing. After? 4 in 5. It’s not magic. It’s just… asking the right way. Showing the list. No judgment. No 'Have you ever…?' Just 'Did you use any of these?' It’s a small change. But it saves lives. I wish every provider had this tool.
APRIL HARRINGTON
March 14, 2026 at 08:29 AM
OMG I just read this and cried in public like a mess but like seriously why is no one talking about how fentanyl is in EVERYTHING now I thought I was taking cocaine but it was probably laced with something that turned my friend blue and now he’s in rehab and I feel so guilty because I didn’t even know what to look for and I just kept saying oh he’s fine he’s fine he’s fine
Neeti Rustagi
March 14, 2026 at 12:22 PM
The scientific rigor of this article is commendable. The data presented, particularly the 10-fold increase in fatal overdose risk when opioids are combined with benzodiazepines, aligns with the 2022 JAMA Internal Medicine findings. Furthermore, the emphasis on non-judgmental inquiry as a clinical intervention is evidence-based and ethically sound. I would only suggest supplementing the self-check tool with mandatory physician training in motivational interviewing, as patient disclosure remains contingent on perceived safety, not merely question phrasing.
Leon Hallal
March 15, 2026 at 22:25 PM
They’re all lying. Every single one. Doctors don’t care. Pharmacies don’t track. The government just wants you to think they’re helping. But the real reason these deaths keep happening? Because they want you scared. Scared enough to stay on the pills. Scared enough to not ask questions. Scared enough to never talk to anyone. That’s how they keep the money flowing. This isn’t about harm reduction. It’s about control.
Stephen Rudd
March 16, 2026 at 14:08 PM
You know what’s really dangerous? People who think they can 'check' interactions with some app. That’s like using a GPS to navigate a warzone. The real problem isn’t the drugs-it’s the cult of self-reliance. You don’t need a checklist. You need a community. You need someone who knows your name and your habits. Not a website. Not a pamphlet. A person. And if you don’t have one? You’re already one step from dead.
Scott Easterling
March 18, 2026 at 03:33 AM
I’ve been following this for years… and I’ve got news for you: the 'Overdose Risk Self-Check' is a scam. It’s built on cherry-picked data. 88% accurate? Where’s the peer review? The CDC doesn’t even endorse it. And 'naloxone on hand'? That’s not prevention-it’s damage control. We’re treating symptoms, not causes. The real solution? Legalize everything. Regulate it. Tax it. Stop criminalizing users. Stop pretending this is about 'safety.' It’s about power.
Judith Manzano
March 20, 2026 at 01:43 AM
I’m so glad this exists. I’ve been helping my dad navigate his pain meds after his back surgery, and I had no idea how dangerous mixing them with his sleep aid was. We checked the tool, talked to his pharmacist, and now he’s on a safer regimen. It’s not glamorous. But it’s quiet, daily courage. And I think that’s where real change happens-not in headlines, but in kitchens, at dinner tables, in quiet conversations that say: 'I’m here. Let’s figure this out together.'
Peter Kovac
March 21, 2026 at 12:10 PM
This article is dangerously oversimplified. You cite studies, but ignore confounding variables. The 75% statistic on polydrug overdoses? It conflates intentional recreational use with accidental interactions. The 90% preventable claim? Based on flawed assumptions about patient compliance. And naloxone? It’s a band-aid. You’re not addressing root causes: poverty, mental health neglect, pharmaceutical marketing. This reads like a PR campaign disguised as public health advice.



Janelle Pearl
March 9, 2026 at 14:28 PM
I’ve seen this play out in my own family. My sister was prescribed oxycodone after surgery and started taking Xanax for anxiety. She didn’t think it was a big deal-'I only take one at a time.' But the night she stopped breathing? It was after a glass of wine. I’ll never forget the sound of the alarm going off at 3 a.m. We got her back with naloxone. She’s sober now. But I wish someone had just asked her: 'What else are you taking?' Not in a judgmental way. Just… plainly.