
Quick Facts You Should Know
You might think you're allergic to penicillin-but here's the kicker: 9 out of 10 people labeled with penicillin allergy don't actually have it. A 2022 CDC report revealed only 1% of Americans truly react dangerously to this common antibiotic. That false label costs billions in healthcare waste and forces patients onto riskier medications.
- Immediate reactions happen within an hour; delayed ones appear days later
- Skin testing + oral challenge removes the label for 90% of "allergic" patients
- Misdiagnosed allergies fuel antibiotic-resistant superbugs like MRSA
What Actually Causes Penicillin Allergies?
Penicillin allergy isn't one single thing-it's your immune system overreacting to the drug's chemical structure. When Alexander Fleming discovered penicillin in 1928, he never imagined how many people would later fear it unnecessarily.The culprit? Beta-lactam ring molecules triggering two distinct reaction types:
| Reaction Type | Timing | Common Symptoms |
|---|---|---|
| Immediate | <1 hour after dose | Hives, throat swelling, breathing trouble |
| Delayed | 72+ hours post-dose | Rash, fever, organ inflammation |
Critical detail: 80% of IgE-mediated allergies fade within a decade without re-exposure. That old childhood rash story? Probably irrelevant today.
Your Reaction Might Not Be an Allergy
Remember that stomach ache after antibiotics? Or mild headache? Those aren't allergies-just side effects. According to Cleveland Clinic data:
- Nausea/vomiting = intolerance, not immune response
- Skin itching alone doesn't equal anaphylaxis risk
- Fever during infection ≠ drug reaction
This distinction matters because low-risk patients can safely take cefazolin (common surgical prophylaxis) without testing. Don't let vague histories limit life-saving treatments.
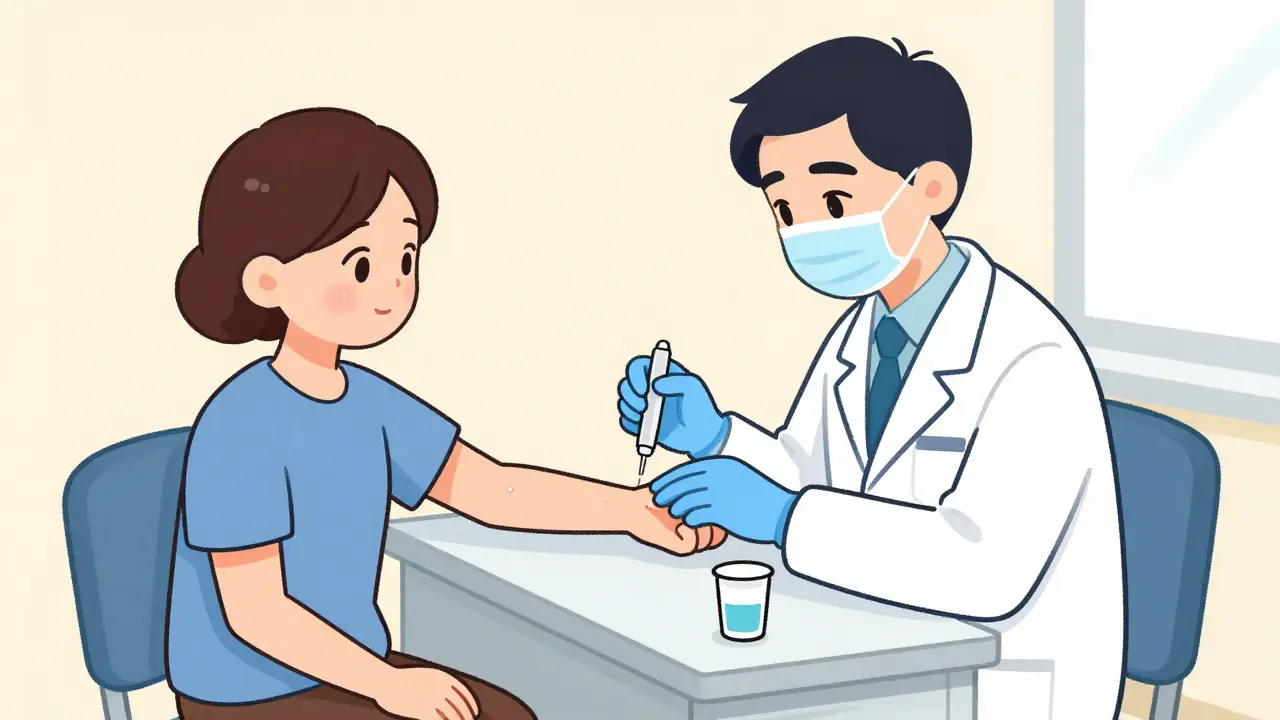
Testing Removes 90% of False Labels
Allergy testing protocol involves two steps backed by CDC standards:- Skin prick test: Tiny amounts of penicillin derivatives applied via needle
- Oral challenge: Supervised amoxicillin dose followed by 1-hour monitoring
Dr. Trevor Van Schooneveld's UNMC team found negative results mean zero anaphylaxis risk. Yet only 15% of eligible patients get tested. Why? Doctors often skip testing due to workflow pressures.
High-Risk Cases Need Special Care
If you experienced life-threatening symptoms before-like tongue swelling requiring epinephrine-that's different. The CDC defines three alert zones:
| Risk Level | History Required | Action Needed |
|---|---|---|
| Low | Vague past reaction >5 years ago | Direct antibiotic challenge safe |
| Moderate | Hives/swelling within 5 years | Allergy specialist referral |
| High | Anaphylaxis/Stevens-Johnson syndrome | Avoid all beta-lactams permanently |
Recent surgery patients face extra danger: Misdiagnosed penicillin allergy increases C. diff infection rates by 35%, per JACI 2019 data.

Protect Yourself With These Steps
Beyond testing, smart documentation saves lives:
- Wear medical alert bracelet for emergency ID clarity
- Update records immediately after successful challenges
- Carry EpiPen if history includes breathing difficulties
Cleveland Clinic warns: Never ignore throat-tightness signs-call emergency services instantly.
The Hidden Cost of Unnecessary Labels
Here's what nobody tells you: False allergy labels drive up antibiotic prices and hospital stays. UCSF researchers tracked $1.2 billion annual US losses from alternative drugs like vancomycin. Even scarier? Broad-spectrum antibiotics fuel resistant bacteria outbreaks.
Orthopedic surgeons report 124 tested patients prevent just one surgical site infection-but that's 124 safer recoveries overall. Imagine if every ER used systematic de-labeling protocols.
Frequent Questions Answered
Can I safely stop wearing my medical alert bracelet after testing?
Yes-if your skin tests and oral challenge were completely negative. Document the date of testing; repeat evaluation needed after 10 years or following severe future reactions.
Why did my doctor refuse cephalosporins despite negative penicillin tests?
Third/fourth-generation cephalosporins carry minimal cross-reactivity (<2%) for non-severe histories. Request specific allergist clearance letter referencing 2022 CDC guidelines.
Is home observation sufficient instead of clinic testing?
Absolutely not. Home settings lack emergency crash carts and rapid IV access required for unexpected anaphylaxis. Always seek supervised clinical environments.
12 Comments
Sabrina Herciu
March 29, 2026 at 09:28 AM
The distinction between immediate and delayed reactions is clinically significant. While anaphylaxis requires epinephrine, rashes appearing later are less severe. Physicians should differentiate based on symptom timing accurately. Skin testing remains the gold standard for diagnosis currently. Oral challenges are supervised under strict medical observation protocols. Documentation in electronic health records must be updated promptly after negative results. Failure to update creates liability issues for future prescribers. Interdisciplinary communication ensures continuity of care across departments.
walker texaxsranger
March 31, 2026 at 05:31 AM
most of this is nonsense regarding immune system reactivity. beta lactam ring instability varies by molecular weight. clinical trials rarely account for genetic polymorphism differences. big pharma pushes cheap drugs to increase volume. regulatory bodies ignore adverse event reporting systematically. cross reactivity rates are understated in literature. do not trust standardized protocols blindly. anecdotal evidence contradicts large scale studies often. stay vigilant regarding synthetic additives. your history matters more than a chart review
Philip Wynkoop
April 1, 2026 at 14:34 PM
I get what you mean but ignoring meds can be dangerous 😬
Rohan Kumar
April 3, 2026 at 10:25 AM
Sure, just let the doctors decide again lol 🙄. They love their billing codes for useless tests anyway. The truth is hidden in plain sight most times 🕵️♂️. Why would hospitals want to save money honestly? Just kidding... maybe 😏. Most people keep the label forever because it is convenient. Insurance loves paying for the expensive stuff instead 🤑. Do not expect much change from this guide tbh. 📉
Eva Maes
April 4, 2026 at 18:25 PM
Your clinical precision misses the broader systemic failure completely. The bureaucracy acts like a malignant tumor consuming resources inefficiently. Standardization becomes a shackle rather than a tool for liberation here. Physicians are merely cogswirls in a mechanistic healthcare machine. Ignoring the socioeconomic barriers renders this advice practically useless for many. Privilege dictates access to specialist referrals constantly. We must dismantle the structural rot before tweaking protocols slightly. Your focus on paperwork obscures the reality of bedside care struggles.
gina macabuhay
April 5, 2026 at 23:54 PM
You are neglecting the moral imperative of public health safety entirely. Individuals who refuse testing endanger their entire community unnecessarily. Ignorance is not an excuse for poor health choices anymore. Responsibility lies with the patient to verify their status correctly. We cannot allow negligence to spread misinformation further. Compliance is non-negotiable for societal stability. Every person must take action regarding their medical history immediately. Hiding behind excuses perpetuates avoidable harm to others. Accountability must be enforced strictly by providers. Standards exist for a reason that benefits everyone collectively.
Monique Louise Hill
April 6, 2026 at 20:17 PM
I agree with the sentiment but we need compassion too 🌸. Fear drives behavior more than guilt does sometimes 😴. People are scared of needles and doctors unfortunately 😿. We should encourage without attacking them so harshly . Everyone makes mistakes in their health journey daily 🚵️. Kindness works better than aggression in changing minds generally 👐. Let us support each other through the testing process kindly 🤗. Love heals more than lectures ever could heal ❤️.
Sarah Klingenberg
April 7, 2026 at 07:54 AM
This is a great reminder for us all to stay informed 🙂. Knowledge empowers patients to speak up confidently. It is okay to feel nervous about medical procedures though 🙂. We can talk to trusted allies for support when needed 🤝. Community understanding grows when we share experiences openly 💬. Remember to check your own records periodically 📋. Small steps lead to big changes in health habits eventually 🚀. You got this no matter what the situation feels like 🌟.
Shawn Sauve
April 8, 2026 at 02:31 AM
Thank you for the kind encouragement here 🙂. It helps to feel supported during stressful health scares 🤗. We should all be grateful for positive voices online 💖. Sharing knowledge builds stronger communities for sure 🌈. Keep spreading that helpful energy always 🌼.
Richard Kubíček
April 8, 2026 at 03:21 AM
There is hope in understanding the science clearly. Misunderstandings fade as education spreads wider across populations. We move forward by learning from past errors honestly. Trust in medicine can be rebuilt through transparency gradually. The future holds promise for safer treatments universally. Humanity thrives when we prioritize accuracy over fear instinctively. This is a step toward a healthier world for children. Progress happens even when slow and difficult initially.
Austin Oguche
April 9, 2026 at 08:09 AM
Cultural sensitivity impacts adherence to testing recommendations globally. Diverse populations may require tailored educational approaches for efficacy. Medical history documentation standards vary regionally significantly. International collaboration improves diagnostic accuracy rates substantially. We must consider local resources when implementing protocols widely. Accessibility determines success more than guidelines alone typically. Informed consent processes protect patient autonomy effectively. Respectful communication bridges gaps between cultures successfully.



Monique Ball
March 28, 2026 at 15:28 PM
This is such a crucial topic for us to discuss today! ✋🤟 So many patients suffer from unnecessary fear because of outdated records. The medical community needs to prioritize these testing protocols much sooner than later. I believe we can improve outcomes significantly if everyone follows the guidelines. It is really frustrating to see how waste accumulates in hospitals. We should advocate for better access to skin prick tests everywhere. My own experience suggests that documentation is often messy. Proper record keeping could save millions annually without fail. 💸 The statistics regarding false labels are truly staggering numbers. Everyone deserves the correct medication during a crisis situation. Avoiding beta-lactams limits treatment options dangerously. It is sad that workflow pressures prevent proper care delivery. We must demand changes from administrative staff immediately. Health insurance companies should cover the challenge procedures fully. 🚣 This way, no one pays out of pocket for life-saving tests. The CDC report was clear about the risks involved with alternatives. Vancomycin carries higher infection rates compared to standard penicillin. 👯️ Resistant bacteria threaten public health significantly in our current climate. I hope this thread raises awareness among general practitioners. We need to update patient files regularly to reflect new test results. Safety must always remain the top priority for every single provider. Thank you for compiling all this useful information together. ❤️